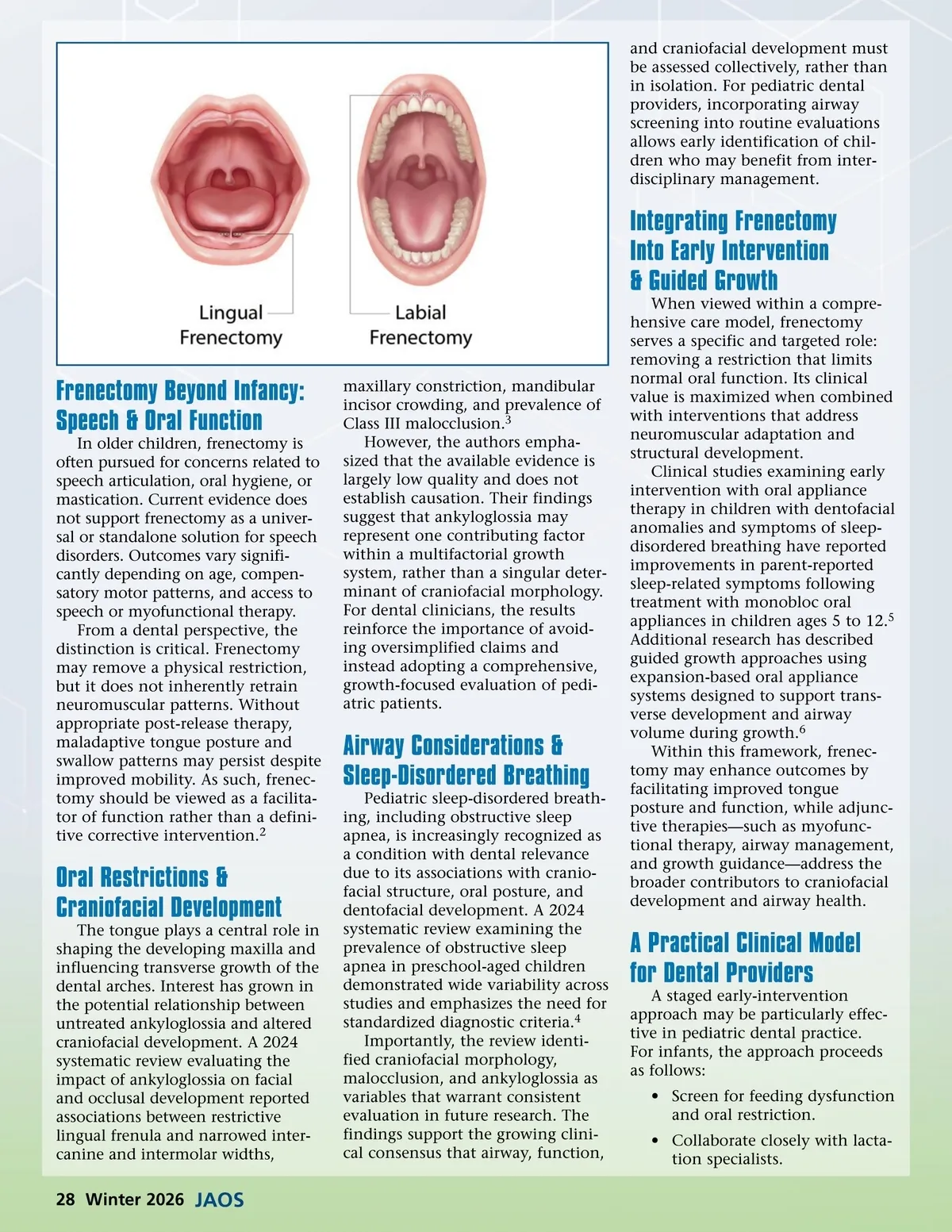
and craniofacial development must be assessed collectively, rather than in isolation. For pediatric dental providers, incorporating airway screening into routine evaluations allows early identification of chil-dren who may benefit from inter-disciplinary management. Integrating Frenectomy Into Early Intervention & Guided Growth When viewed within a compre-hensive care model, frenectomy serves a specific and targeted role: removing a restriction that limits normal oral function. Its clinical value is maximized when combined with interventions that address neuromuscular adaptation and structural development. Clinical studies examining early intervention with oral appliance therapy in children with dentofacial anomalies and symptoms of sleep-disordered breathing have reported improvements in parent-reported sleep-related symptoms following treatment with monobloc oral appliances in children ages 5 to 12. 5 Additional research has described guided growth approaches using expansion-based oral appliance systems designed to support trans-verse development and airway volume during growth. 6 Within this framework, frenec-tomy may enhance outcomes by facilitating improved tongue posture and function, while adjunc-tive therapies—such as myofunc-tional therapy, airway management, and growth guidance—address the broader contributors to craniofacial development and airway health. Frenectomy Beyond Infancy: Speech & Oral Function In older children, frenectomy is often pursued for concerns related to speech articulation, oral hygiene, or mastication. Current evidence does not support frenectomy as a univer-sal or standalone solution for speech disorders. Outcomes vary signifi-cantly depending on age, compen-satory motor patterns, and access to speech or myofunctional therapy. From a dental perspective, the distinction is critical. Frenectomy may remove a physical restriction, but it does not inherently retrain neuromuscular patterns. Without appropriate post-release therapy, maladaptive tongue posture and swallow patterns may persist despite improved mobility. As such, frenec-tomy should be viewed as a facilita-tor of function rather than a defini-tive corrective intervention. 2 maxillary constriction, mandibular incisor crowding, and prevalence of Class III malocclusion. 3 However, the authors empha-sized that the available evidence is largely low quality and does not establish causation. Their findings suggest that ankyloglossia may represent one contributing factor within a multifactorial growth system, rather than a singular deter-minant of craniofacial morphology. For dental clinicians, the results reinforce the importance of avoid-ing oversimplified claims and instead adopting a comprehensive, growth-focused evaluation of pedi-atric patients. Airway Considerations & Sleep-Disordered Breathing Pediatric sleep-disordered breath-ing, including obstructive sleep apnea, is increasingly recognized as a condition with dental relevance due to its associations with cranio-facial structure, oral posture, and dentofacial development. A 2024 systematic review examining the prevalence of obstructive sleep apnea in preschool-aged children demonstrated wide variability across studies and emphasizes the need for standardized diagnostic criteria. 4 Importantly, the review identi-fied craniofacial morphology, malocclusion, and ankyloglossia as variables that warrant consistent evaluation in future research. The findings support the growing clini-cal consensus that airway, function, Oral Restrictions & Craniofacial Development The tongue plays a central role in shaping the developing maxilla and influencing transverse growth of the dental arches. Interest has grown in the potential relationship between untreated ankyloglossia and altered craniofacial development. A 2024 systematic review evaluating the impact of ankyloglossia on facial and occlusal development reported associations between restrictive lingual frenula and narrowed inter-canine and intermolar widths, A Practical Clinical Model for Dental Providers A staged early-intervention approach may be particularly effec-tive in pediatric dental practice. For infants, the approach proceeds as follows: • Screen for feeding dysfunction and oral restriction. • Collaborate closely with lacta-tion specialists. 28 Winter 2026 JAOS
Journal of the American Orthodontic Society Winter 2026: Page 28