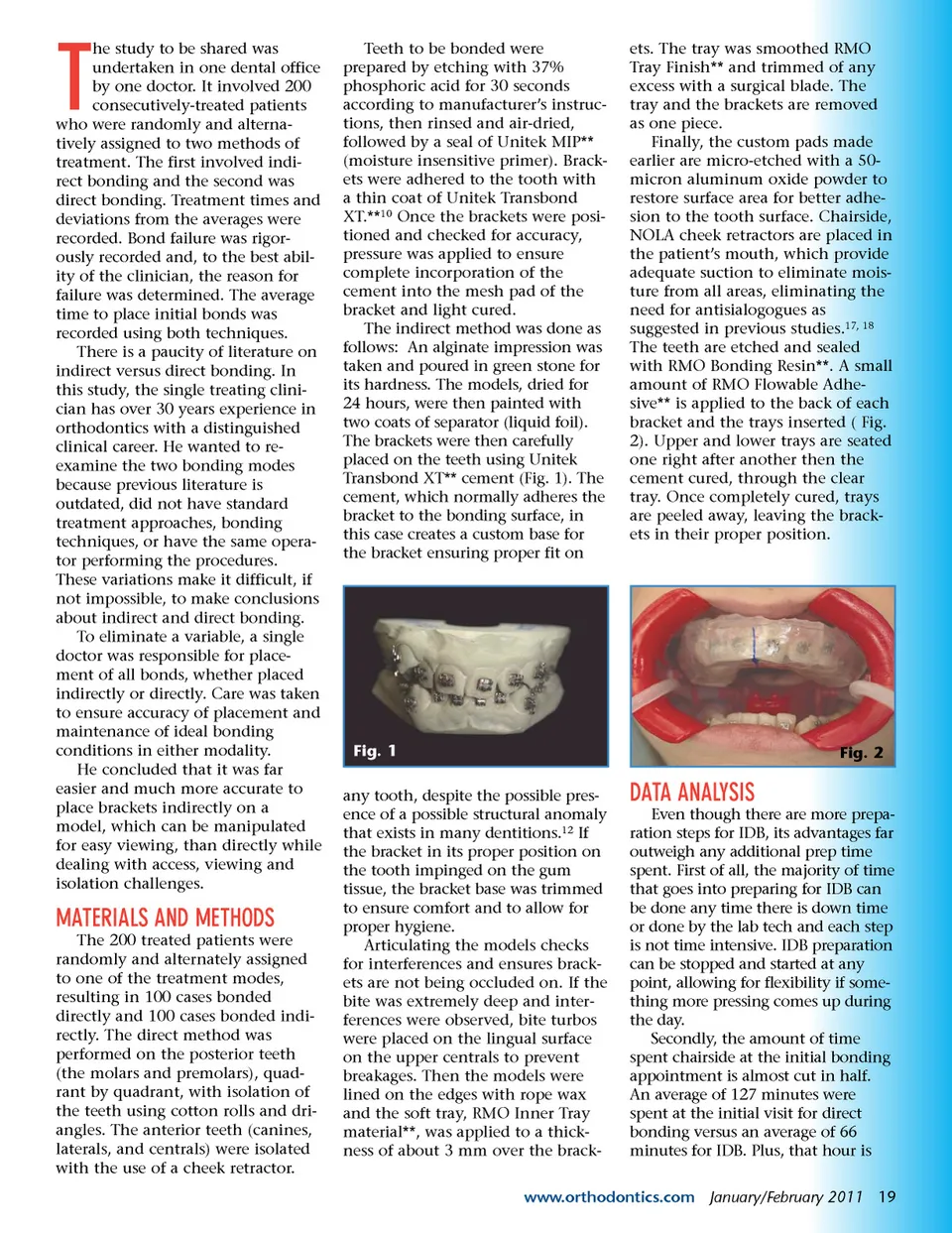
he study to be shared was undertaken in one dental office by one doctor. It involved 200 consecutively-treated patients who were randomly and alterna-tively assigned to two methods of treatment. The first involved indi-rect bonding and the second was direct bonding. Treatment times and deviations from the averages were recorded. Bond failure was rigor-ously recorded and, to the best abil-ity of the clinician, the reason for failure was determined. The average time to place initial bonds was recorded using both techniques. There is a paucity of literature on indirect versus direct bonding. In this study, the single treating clini-cian has over 30 years experience in orthodontics with a distinguished clinical career. He wanted to re-examine the two bonding modes because previous literature is outdated, did not have standard treatment approaches, bonding techniques, or have the same opera-tor performing the procedures. These variations make it difficult, if not impossible, to make conclusions about indirect and direct bonding. To eliminate a variable, a single doctor was responsible for place-ment of all bonds, whether placed indirectly or directly. Care was taken to ensure accuracy of placement and maintenance of ideal bonding conditions in either modality. He concluded that it was far easier and much more accurate to place brackets indirectly on a model, which can be manipulated for easy viewing, than directly while dealing with access, viewing and isolation challenges. T Teeth to be bonded were prepared by etching with 37% phosphoric acid for 30 seconds according to manufacturer’s instruc-tions, then rinsed and air-dried, followed by a seal of Unitek MIP** (moisture insensitive primer). Brack-ets were adhered to the tooth with a thin coat of Unitek Transbond XT.** 10 Once the brackets were posi-tioned and checked for accuracy, pressure was applied to ensure complete incorporation of the cement into the mesh pad of the bracket and light cured. The indirect method was done as follows: An alginate impression was taken and poured in green stone for its hardness. The models, dried for 24 hours, were then painted with two coats of separator (liquid foil). The brackets were then carefully placed on the teeth using Unitek Transbond XT** cement (Fig. 1). The cement, which normally adheres the bracket to the bonding surface, in this case creates a custom base for the bracket ensuring proper fit on ets. The tray was smoothed RMO Tray Finish** and trimmed of any excess with a surgical blade. The tray and the brackets are removed as one piece. Finally, the custom pads made earlier are micro-etched with a 50-micron aluminum oxide powder to restore surface area for better adhe-sion to the tooth surface. Chairside, NOLA cheek retractors are placed in the patient’s mouth, which provide adequate suction to eliminate mois-ture from all areas, eliminating the need for antisialogogues as suggested in previous studies. 17, 18 The teeth are etched and sealed with RMO Bonding Resin**. A small amount of RMO Flowable Adhe-sive** is applied to the back of each bracket and the trays inserted ( Fig. 2). Upper and lower trays are seated one right after another then the cement cured, through the clear tray. Once completely cured, trays are peeled away, leaving the brack-ets in their proper position. Fig. 1 any tooth, despite the possible pres-ence of a possible structural anomaly that exists in many dentitions. 12 If the bracket in its proper position on the tooth impinged on the gum tissue, the bracket base was trimmed to ensure comfort and to allow for proper hygiene. Articulating the models checks for interferences and ensures brack-ets are not being occluded on. If the bite was extremely deep and inter-ferences were observed, bite turbos were placed on the lingual surface on the upper centrals to prevent breakages. Then the models were lined on the edges with rope wax and the soft tray, RMO Inner Tray material**, was applied to a thick-ness of about 3 mm over the brack-Fig. 2 DATA ANALYSIS Even though there are more prepa-ration steps for IDB, its advantages far outweigh any additional prep time spent. First of all, the majority of time that goes into preparing for IDB can be done any time there is down time or done by the lab tech and each step is not time intensive. IDB preparation can be stopped and started at any point, allowing for flexibility if some-thing more pressing comes up during the day. Secondly, the amount of time spent chairside at the initial bonding appointment is almost cut in half. An average of 127 minutes were spent at the initial visit for direct bonding versus an average of 66 minutes for IDB. Plus, that hour is MATERIALS AND METHODS The 200 treated patients were randomly and alternately assigned to one of the treatment modes, resulting in 100 cases bonded directly and 100 cases bonded indi-rectly. The direct method was performed on the posterior teeth (the molars and premolars), quad-rant by quadrant, with isolation of the teeth using cotton rolls and dri-angles. The anterior teeth (canines, laterals, and centrals) were isolated with the use of a cheek retractor. www.orthodontics.com January/February 2011 19
Journal of the American Orthodontic Society January - February 2011: Page 19