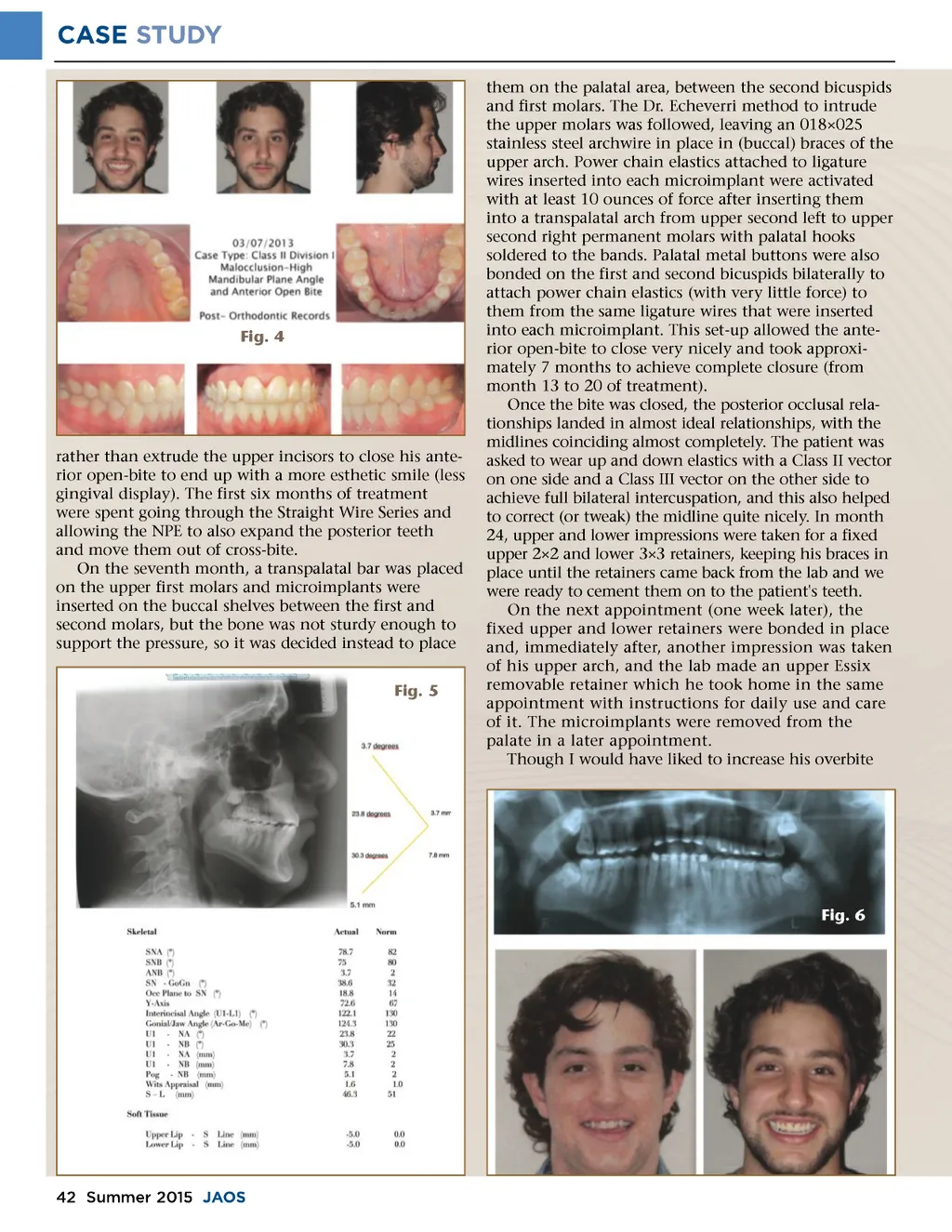
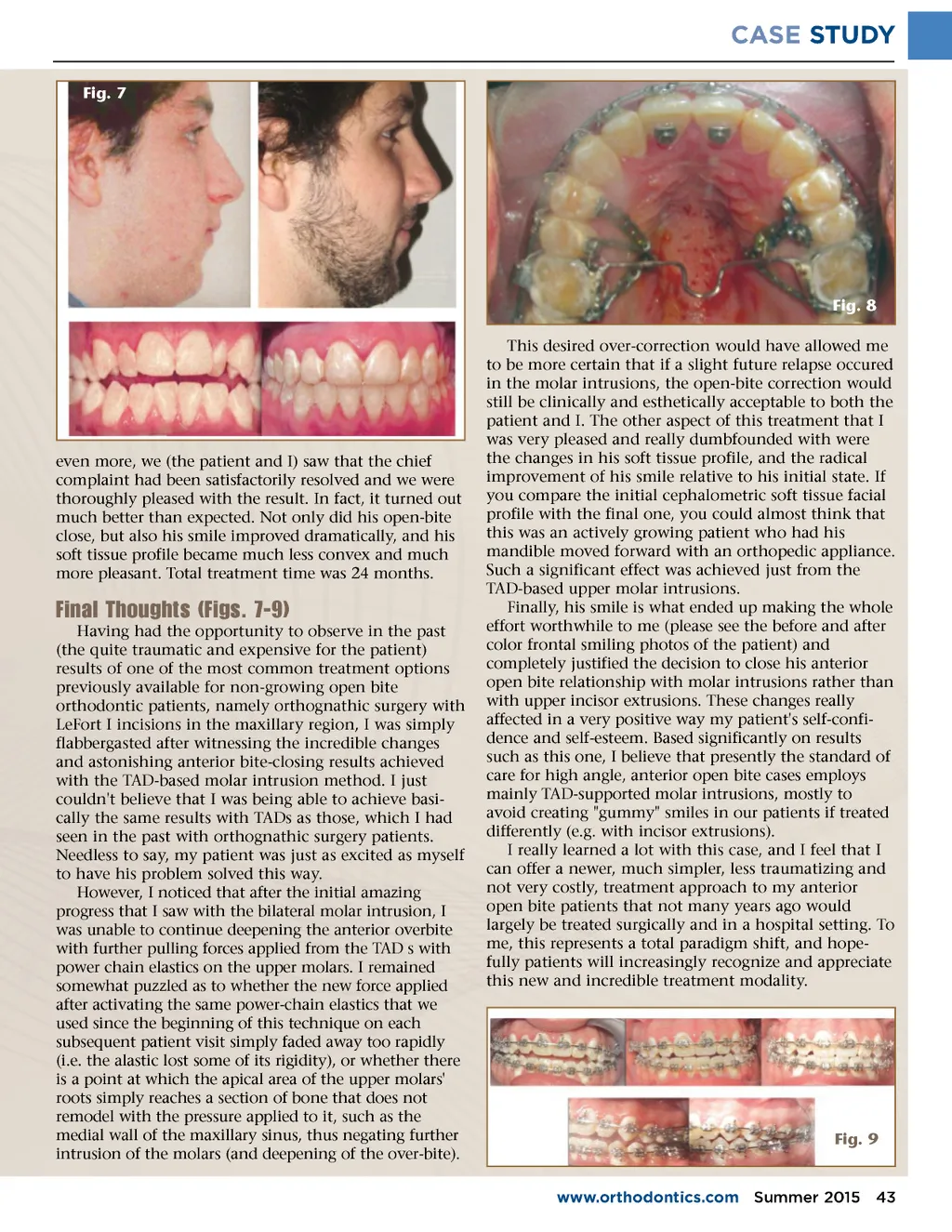
CASE STUDY Fig. 7 Fig. 8 This desired over-correction would have allowed me to be more certain that if a slight future relapse occured in the molar intrusions, the open-bite correction would still be clinically and esthetically acceptable to both the patient and I. The other aspect of this treatment that I was very pleased and really dumbfounded with were the changes in his soft tissue profile, and the radical improvement of his smile relative to his initial state. If you compare the initial cephalometric soft tissue facial profile with the final one, you could almost think that this was an actively growing patient who had his mandible moved forward with an orthopedic appliance. Such a significant effect was achieved just from the TAD-based upper molar intrusions. Finally, his smile is what ended up making the whole effort worthwhile to me (please see the before and after color frontal smiling photos of the patient) and completely justified the decision to close his anterior open bite relationship with molar intrusions rather than with upper incisor extrusions. These changes really affected in a very positive way my patient's self-confi-dence and self-esteem. Based significantly on results such as this one, I believe that presently the standard of care for high angle, anterior open bite cases employs mainly TAD-supported molar intrusions, mostly to avoid creating "gummy" smiles in our patients if treated differently (e.g. with incisor extrusions). I really learned a lot with this case, and I feel that I can offer a newer, much simpler, less traumatizing and not very costly, treatment approach to my anterior open bite patients that not many years ago would largely be treated surgically and in a hospital setting. To me, this represents a total paradigm shift, and hope-fully patients will increasingly recognize and appreciate this new and incredible treatment modality. even more, we (the patient and I) saw that the chief complaint had been satisfactorily resolved and we were thoroughly pleased with the result. In fact, it turned out much better than expected. Not only did his open-bite close, but also his smile improved dramatically, and his soft tissue profile became much less convex and much more pleasant. Total treatment time was 24 months. Final Thoughts (Figs. 7-9) Having had the opportunity to observe in the past (the quite traumatic and expensive for the patient) results of one of the most common treatment options previously available for non-growing open bite orthodontic patients, namely orthognathic surgery with LeFort I incisions in the maxillary region, I was simply flabbergasted after witnessing the incredible changes and astonishing anterior bite-closing results achieved with the TAD-based molar intrusion method. I just couldn't believe that I was being able to achieve basi-cally the same results with TADs as those, which I had seen in the past with orthognathic surgery patients. Needless to say, my patient was just as excited as myself to have his problem solved this way. However, I noticed that after the initial amazing progress that I saw with the bilateral molar intrusion, I was unable to continue deepening the anterior overbite with further pulling forces applied from the TAD s with power chain elastics on the upper molars. I remained somewhat puzzled as to whether the new force applied after activating the same power-chain elastics that we used since the beginning of this technique on each subsequent patient visit simply faded away too rapidly (i.e. the alastic lost some of its rigidity), or whether there is a point at which the apical area of the upper molars' roots simply reaches a section of bone that does not remodel with the pressure applied to it, such as the medial wall of the maxillary sinus, thus negating further intrusion of the molars (and deepening of the over-bite). Fig. 9 www.orthodontics.com Summer 2015 43
Journal of the American Orthodontic Society Summer 2015-Buyer's Guide: Page 43